
Low Complexity IVF is a streamlined form of IVF designed as a middle step between IUI and conventional IVF. It uses core IVF technology—retrieving eggs and fertilizing them in the lab—but simplifies the medication plan and avoids many add-ons that aren’t needed for every patient. At Hanabusa IVF, Low Complexity IVF is a thoughtful option for patients who want a more effective step than IUI, with a lower medication burden and a simpler overall experience when the clinical picture supports it.
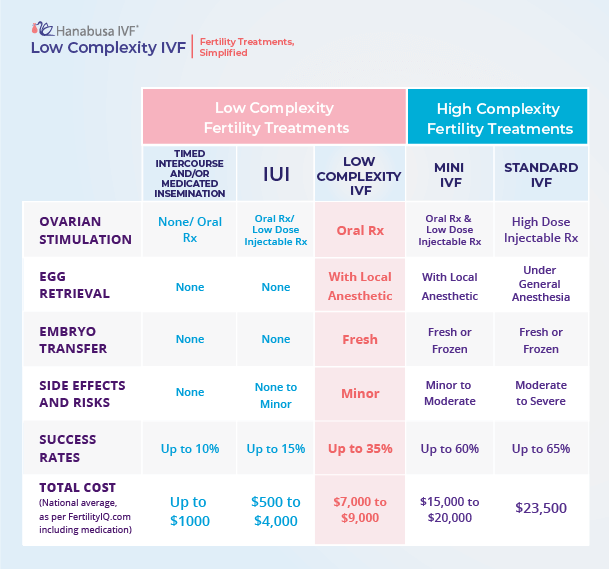

Not everyone needs the most complex version of IVF. We match treatment intensity to your biology—so you can pursue IVF technology with a simpler plan when it’s medically appropriate.
Often oral medication–based stimulation designed to reduce injections and side effects while supporting a meaningful response.
We set expectations early about who this is for—and when moving to Mini IVF or conventional IVF is a better next step.
When appropriate, retrieval can be designed with a lower-intervention anesthesia plan to reduce burden and recovery time.
We use IVF fundamentals thoughtfully and avoid “extras by default,” while still recommending ICSI, freezing, or testing when clinically indicated.
If Low Complexity IVF isn’t enough, you’re already in a system built for personalized IVF strategy—without starting over.
A simpler, lower-burden IVF approach designed to reduce unnecessary steps and medication—while keeping the plan personalized to your body and goals.

Review your goals, timeline, and diagnosis
Confirm this is the right-fit pathway (straightforward factors, no major complexity flags)
Align on priorities: comfort, efficiency, embryo goals, and transfer strategy
Baseline ultrasound (AFC, ovaries, uterine lining/structure check)
Baseline labs to confirm readiness and guide safe timing
Any required pre-treatment safety checks based on your plan
Build a streamlined stimulation plan (often with lower medication than typical “high-dose” approaches)
Set a simple monitoring schedule with clear decision points
Confirm trigger strategy and retrieval timing plan
Start stimulation medications as prescribed
Ultrasounds (and labs as needed) to track follicle growth and adjust timing/dose
Keep monitoring efficient while ensuring precision
Trigger timed to optimize egg maturity
Outpatient egg retrieval performed on schedule
Fertilization via IVF or ICSI as indicated
Embryo culture and development tracking
Decide whether to culture to blastocyst based on your embryo plan
Plan transfer timing based on uterine readiness and embryo stage
Freeze embryos when it improves the uterine environment or supports better timing
Single embryo transfer planning when transfer is the next best step

For some patients, IUI doesn’t go far enough—yet conventional IVF may be more intervention than needed. Low Complexity IVF can offer a meaningful step up in effectiveness with fewer medications and a simpler approach, while still using IVF lab technology to help fertilization and embryo development happen under controlled conditions.

You want a step between IUI and conventional IVF based on your evaluation
You prefer fewer injections and a lower-medication approach (when appropriate)
You’ve had unsuccessful IUIs and want a more effective next step
You’re expected to respond reasonably well to a gentler stimulation plan
You want IVF technology with a streamlined experience
You have diminished ovarian reserve (DOR) or a history of low response where Mini IVF or specialized protocols may fit better
You need embryo banking, PGT, or a freeze-all strategy based on your goals/diagnosis
You have significant male factor where ICSI is likely needed (we’ll guide you)
Your case suggests conventional IVF would be more efficient from the start


Monitoring frequency (ultrasounds + labs)
Medication plan (often lower medication cost than injectable-heavy protocols, but varies)
Retrieval and anesthesia approach
Lab services needed (standard IVF vs. ICSI when indicated)
Whether freezing, storage, or genetic testing is recommended (case dependent)
Often included: retrieval + basic embryology/lab services and embryo culture through transfer timing
Often separate: medications, some labs/ultrasounds, anesthesia fees, ICSI (if needed), embryo freezing/storage, PGT testing


Success varies widely and depends on diagnosis, age, sperm factors, and how your ovaries respond. The most important factor is whether Low Complexity IVF is the right match for your biology—and whether the plan is adjusted based on real-time response.
Age and ovarian reserve
Diagnosis (unexplained infertility, ovulatory factors, mild male factor, etc.)
Follicle response to oral stimulation
Sperm parameters and fertilization method
Uterine and lining factors
Transfer timing and embryo development

Similar overall timeline to IVF, with a simplified medication plan
Monitoring visits to guide timing and response
Often oral stimulation; some patients may still need tailored support (case dependent)
Outpatient procedure with recovery guidance
Typically a short, in-office procedure with clear next-step instructions
Low Complexity IVF is a streamlined form of IVF that uses core IVF technology with a simpler medication and procedure approach when appropriate—often positioned between IUI and conventional IVF.
IUI places sperm in the uterus around ovulation. Low Complexity IVF retrieves eggs and fertilizes them in the lab—providing more control over fertilization and early embryo development.
Both aim to reduce medication burden, but the best fit depends on your ovarian reserve, response patterns, and goals. We’ll recommend the option that best matches your biology.
Often fewer. Many Low Complexity IVF plans emphasize oral medications, but exact medication needs vary by patient and response.
Not always. The goal is to avoid add-ons by default, but we may recommend ICSI, freezing, or PGT when it improves outcomes or fits your clinical situation.
It can be—especially when you need a step up in effectiveness but may not need the most intensive IVF approach. Your evaluation will guide this.
It can be, especially if medication needs and lab add-ons are lower. Total cost depends on monitoring, anesthesia, and whether additional lab services are indicated.
Some patients benefit more from other strategies—such as significant male factor needing ICSI, uterine factors requiring treatment first, or low reserve cases better served by specialized protocols.
.png)
.png)
.png)
.png)
.png)
.png)
You’re a fit for Traditional Fertility Care if any of these statements resonate with you:
You’re just getting started
You want clear first steps
You’ve explored clinics, but still feel at the beginning
You need fertility testing
Your labs look reassuring
Your situation feels straightforward
You have fewer complicating factors
You’re considering IUI
You’re new to IVF
You’re planning an FET
You’re considering PGT
If anything, complex becomes evident, we smoothly upgrade your pathway.
You’re a fit for Complex Care if any of these statements resonate with you:
Low AMH/AFC or DOR concerns
You have Diminished Ovarian Reserve (DOR)
You have POI or high FSH concerns
You’re considering Ovarian Rejuvenation (PRP)
Age 40+ or time feels limited
Prior IVF didn’t respond as hoped
Low egg numbers / embryo growth issues
Unsuccessful embryo transfers
Recurrent pregnancy loss (2+ losses)
Male factor needs ICSI or TESE
You’ve been told your case is complex
If your case is complex from the start, we build the right strategy from day one.